(Press release sent to media on September 27, 2020)
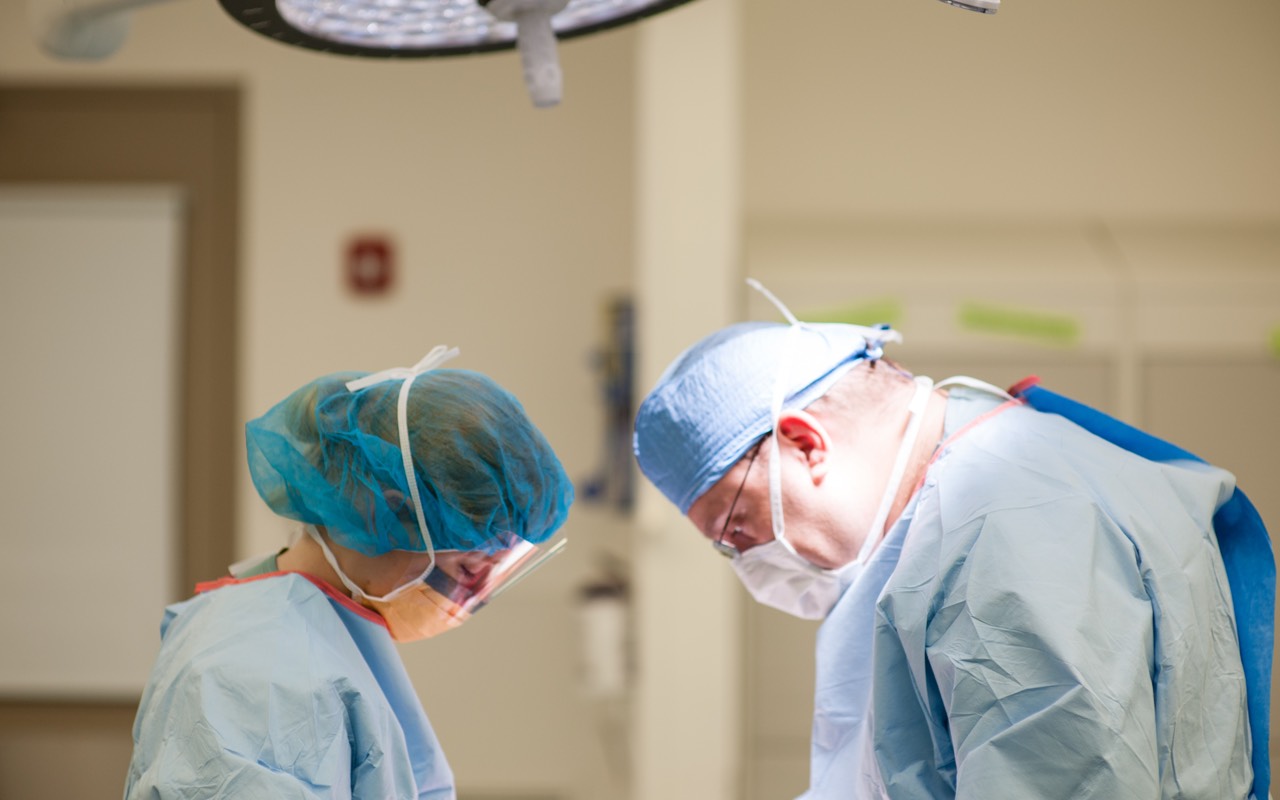
As the 26th anniversary of the shooting death of my small son approaches (Nicholas Green, a seven-year old American boy on holiday in Italy was shot during an attempted robbery on September 29, 1994, died on October 1 and his organs and corneas were donated to seven people, four of them teenagers) Italy is on the verge of making the biggest change in how organ donor families and their recipients are treated since 1999.
A group of legislators in Italy has introduced a bill to allow the two sides to write to each other, if both want to, and eventually meet.
In an exchange of emails between Dr. Pierpaolo Sileri, the Deputy Minister of Health, and myself he today made this unambiguous statement of support for a change in the law. “The liberalization of the contacts between recipients and donor families is a deed of humanity and civilization, a right and proper act that must find its rightful position in a modification of the current legislation, the law 91/99. This battle can and must be driven forward“.
In 2016 when I started this campaign with just one friend, Andrea Scarabelli from Rome, no one supported us. The opposition was so strong we called ourselves Don Quixote and Sancho Panza.
The dramatic change has happened because the media publicized our arguments and ordinary Italians saw the insensitivity, even cruelty, of the current law that effectively prevents the two sides in a transplant from knowing anything but the most basic facts about each other. Donor families don’t even know if their loved one’s recipients are still alive. Recipients can’t thank the people who rescued them when no one else could. Neither side can even send anonymous letters to the other, however much both want to.
 (An article about the Letter to the Italians published by the Italian national newspaper ‘Il Corriere della Sera’)
(An article about the Letter to the Italians published by the Italian national newspaper ‘Il Corriere della Sera’)
In 2016 the whole subject was taboo. Now people all over Italy are asking, ‘If two families with a bond as profound as this want to contact each other why should some bureaucrat be able to say no?’ Feelings like this (for example, one bereaved father, Marco Galbiati of Lecco collected 50,000 signatures calling for a change in the law when his 15-year old son, Ricky, died in 2017) and pressure from the media forced the National Transplant Center to refer the subject to the National Bioethics Committee.
But before proposing a change in the law committee members needed to see hard evidence, not just strong personal feelings. To them we sent data showing that in the United States tens of thousands of transplant families have written to each other and a minority of them have met. In the great majority of cases, the health authorities say, the results have helped the happiness and health of both sides.
After careful consideration, the Committee concluded that the liberalization of the communications was possible, on the lines we proposed, a huge breakthrough. Dr. Carlo Petrini, the National Institute of Health representative on the committee, later described the hard evidence we presented as “a major if not decisive” reason for their recommendation.
That surprise decision has persuaded many other eminent names to support our cause. Donor families may soon have the opportunity to end a lifetime of uncertainty by hearing directly from people whose lives they saved.
There is no feeling quite like contacting your loved one’s recipients: amazement that people whose lives were coming an end are now playing sports, starting careers and having babies, pride that you turned outward to help others when the pressure to turn inward in grief and despair was almost overwhelming and comfort that someone you loved has done so much to make the world a better place. I hope the bill will be passed with widespread support.”
Here is the full statement by Sen. Dr. Pierpaolo Sileri, Deputy Minister of Health in Italy:
“The liberalization of the contacts between recipients and donor families is a deed of humanity and civilization, a right and proper act that must find its rightful position in a modification of the current legislation, the law 91/99. This battle can and must be driven forward, creating a structured system that, beyond the law, can guide recipients and donor families through their grief process. I want to thank once again Nicholas’ family who, without their faith in humanity and will to contribute to our emancipation as persons, wouldn’t have ever pursued the path of the gift and the campaign for a liberalization. It means having your neighbor at heart and waging a battle like Don Quixote, as Reg Green, Nicholas’ father, says in his own words. I know very well the battles against the windmills and I want to support in a productive way and manus legis (through the law) a modification of the 91/99 law – a law that by now is outdated/obsolete. Together we are stronger and more human, as Nicholas and his family taught us.”