Link: https://www.latimes.com/opinion/story/2019-09-27/nicholas-effect-organ-donation-italy
Article by Reg Green
Opinion: ‘The Nicholas Effect’ 25 years later: After we donated our son’s organs, Italy was never the same
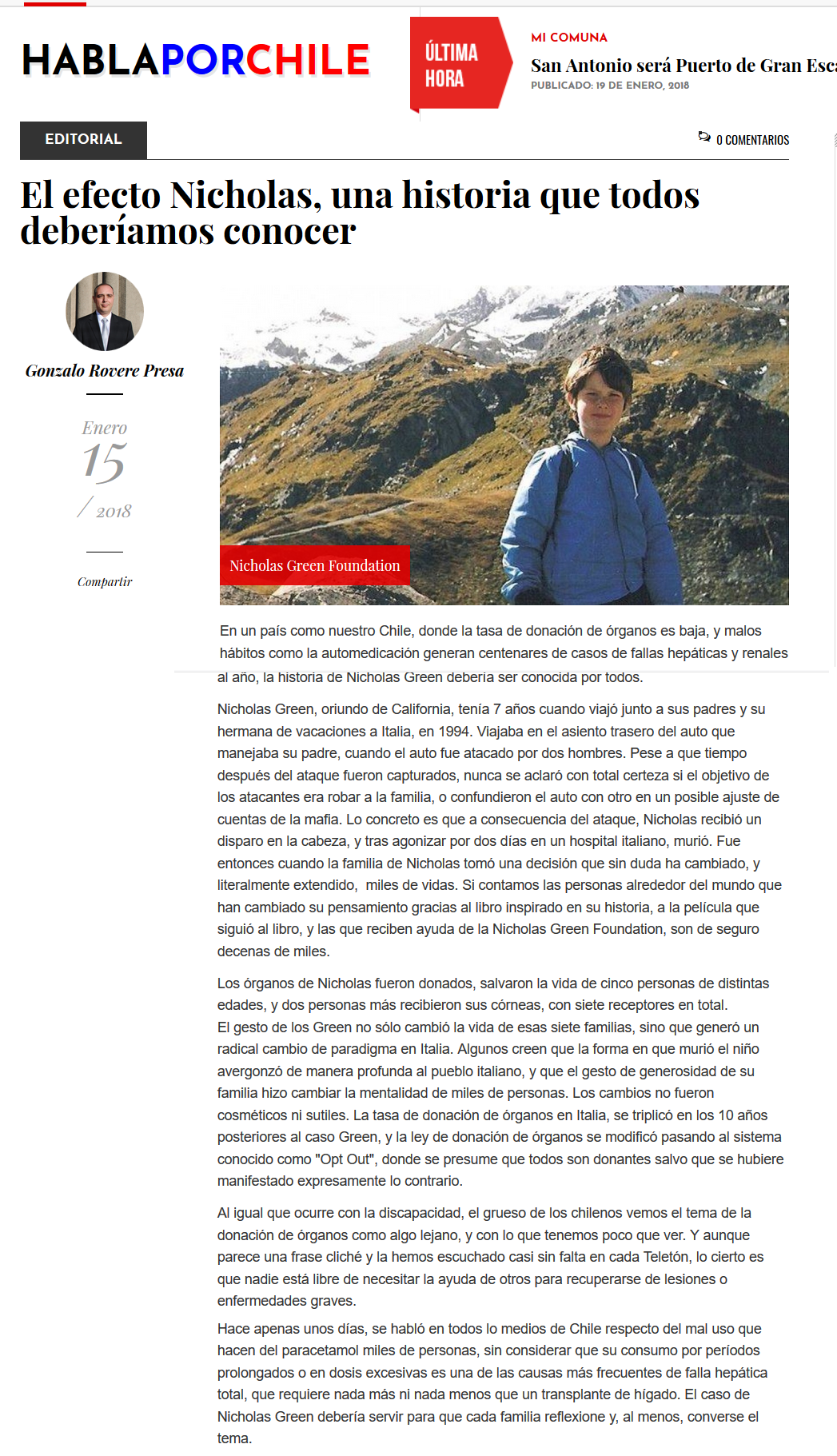
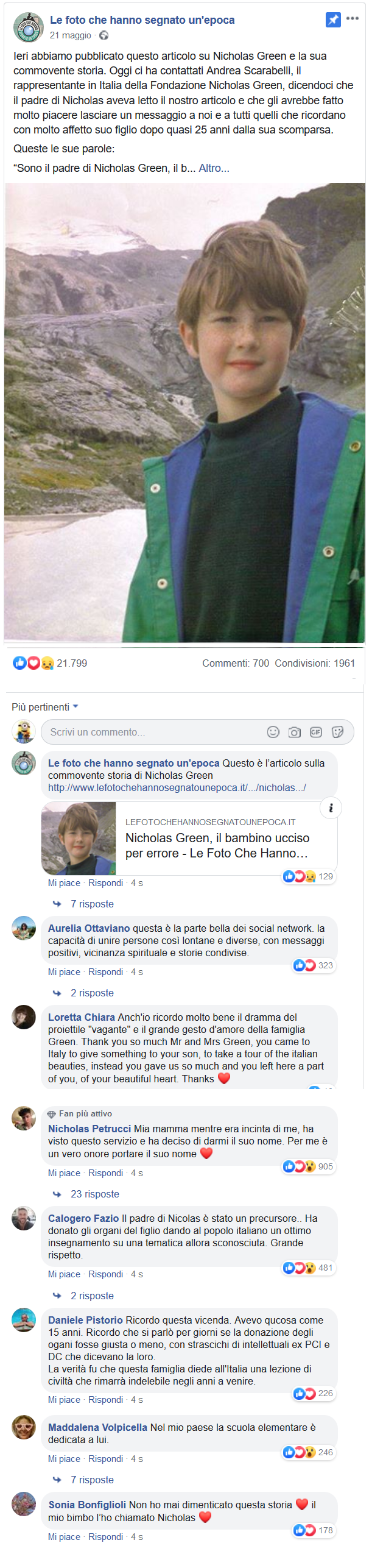
You may remember the story of how my young son, Nicholas, was killed. Many people do.
My wife, Maggie, and I and our two children were on vacation, traveling at night on a divided highway in southern Italy when a car with two masked men pulled up alongside us. One waved a pistol and yelled at us to stop.
We got away — but not before they fired several shots. One hit 7-year-old Nicholas in the head. Mercifully, his 4-year-old sister, Eleanor, asleep beside him, was unhurt.
Later we would learn that the assailants had planned to rob us, mistaking our rented car with its Rome license plates for one delivering jewelry.
For two dreadful days Nicholas was in a coma. He was then declared brain dead. He died 25 years ago Oct. 1.
Since that day, of course, nothing has been the same. I have never again tousled his hair or heard him say, “Good night, Daddy.”
Our only solace is the decision we made to donate his organs and corneas. They went to five terminally ill Italians — some on the edge of death, four of them teenagers — and to two adults who were going blind.
Five of the recipients are still alive.
Nicholas’ heart would beat in the chest of another for 23 years. When the 15-year-old boy received it, he barely had the strength to walk across a room.
The far-reaching and long-lived consequences of our decision to donate his organs have astonished us.
In the 10 years following Nicholas’ death, the rate of organ donation in Italy tripled. No other country has come anywhere near that growth rate. The phenomenon was given a name: the Nicholas Effect.
Letters arrived from all over the world and every corner of society, from admirals and pacifists, football players and gardeners. Believers saw the hand of God and nonbelievers the power of humanity. Young children, who do not even know what a transplant is, know that a little boy did something good and they want to do something good too. The elderly are thrilled to learn they can still do something that important.
Dr. Tom Starzl, often referred to as “the father of transplantation,” wrote to say, “you and your family have done more for organ donation than anyone else I know.” People around the world were suddenly aware that if someone they loved died of a brain injury, they could save three or four families on average from devastation by choosing to give.
Almost immediately after Nicholas was killed, a town in Sicily named a prominent square after him. What an honor, we thought. But that was just the beginning. More than a hundred streets, parks, playgrounds, bicycle paths and my favorite, a bridge, are named for Nicholas. We are no longer surprised when young men and women step out of a crowd to say they went to the Nicholas Green school in that town.
Maria Pia Pedala was 19 years old and in a coma when she received his liver. She quickly regained health, married and four years later had a baby boy. She named him Nicholas. Now tall and handsome, he is fit enough in a family with a history of liver disease to have been accepted for training as a noncommissioned officer in the Italian navy.
Italian families still name their children after Nicholas, and with the American spelling instead of the traditional Nicolas. I always hope people they meet will ask them how they got their names.
We did interviews everywhere — with Oprah Winfrey, Buddhist television stations in Taiwan, radio stations in Venezuela, magazines in Poland and so on. We wrote articles that appeared in publications such as the Journal of the American Medical Association, the Times of India, Boys’ Life and major newspapers.
So that I would never forget everything that happened — and to encourage other families to donate organs — I wrote a book called “The Nicholas Effect.” It was the basis for a late 1990s made-for-television movie, “Nicholas’ Gift,” starring Jamie Lee Curtis, that has been viewed by tens of millions of people worldwide. I can’t see how anyone can watch that movie and remain indifferent to organ donation.
At the Winter World Transplant Games, an Olympic-type event open only to organ recipients, children from around the world compete in an event called the Nicholas Cup. They learn to race in a week, often with a panache that seems almost lordly given their previous conditions. It’s one more lesson that a transplant does not just prolong life but transforms it.
In almost every country, donated organs fall short of the need. Every day in the U.S., 20 people die waiting for a transplant. Yet everywhere there is a disparity between people who say they are in favor of donating and those who actually do. It’s understandable. These families are coping with sudden death — from a car accident, violence, a stroke — and must make a decision there and then about an issue they probably have never seriously thought about. For many it is just too much.
Saving lives is the most obvious result of any decision to donate. But there are less tangible benefits that testify to the strength of the human spirit. Organ donation leaps the barriers between us: The hearts of black women beat inside white women — and vice versa. Muslims are breathing through Jewish lungs — and vice versa. And, as I always like to remind audiences, some Republicans now see the world through Democratic corneas — and vice versa.
One young woman in Rome wrote to us not long after we lost Nicholas. “Since your son has died my heart is beating faster,” she said. “I now think people, common persons, can change the world. When you go to the little graveyard place, please say this to him. ‘They closed your eyes but you opened mine.’ ”
When I am missing Nicholas more than usual, I like to think of sentiments like that.
Reg Green, 90, is author of “The Nicholas Effect” and advocates for organ donation as president of the Nicholas Green Foundation.
The article on the Facebook page of the L.A. Times: https://www.facebook.com/5863113009/posts/10157950555128010/